Where was I? Oh yes, utterly deflated. Late Saturday night, we went to Publix to buy groceries. I had clipped all the coupons already so I had to go. Right, coupon moms? Then I stayed up too late. And went to sleep listening to a Hypnobabies script. During the night, I felt pressure waves come and go but ignored them. At 6am, I thought I might time a couple–10 minutes apart. No big deal then. I listened to another script. Around 7:45, Scott brought a warm rice sock and turned on some Fleet Foxes. What a nice way to wake.
At 9am, it was like someone flipped a switch. I was making breakfast when the pressure waves went from 10 minutes apart to a very serious 3 minutes apart. The energy changed and I told Scott I was having a baby today. I managed to eat my eggs and toast while standing and rocking. Again, I noticed how much I was thinking like a doula. What position should I take? Should Scott sift me? What about belly-lifting? Do I need to do the rotisserie? Argh, the voice in my head!
Then, without thinking, with the next pressure wave, I began reciting T.S. Eliot’s “The Love Song of J. Alfred Prufrock.” Yes, a poem about a balding man’s mid-life crisis. Yes, that is the focal point I chose folks. Not a nice Psalm. Not a beautiful song. Not even a poet like Neruda or Rilke. I could recite to line 22 (“curled once about the house, and fell asleep”) before the wave ended. I did not feel pain just an intense squeezing sensation.
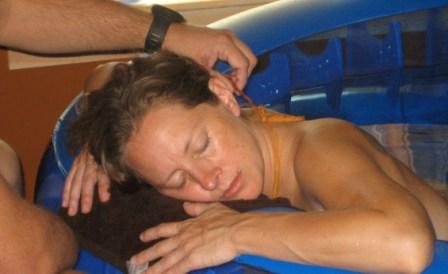 At 10:35am, Scott wrote in the birth log that I said a horrible curse word. Friends–brace yourself. At the end of a pressure wave during which I forgot the words to my poem, I said “Dad-gum.” Time to get into the birth tub. Ah, the birth tub. Bliss. I could drape over the sides and flip my Hypnobabies light switch to “off.”
At 10:35am, Scott wrote in the birth log that I said a horrible curse word. Friends–brace yourself. At the end of a pressure wave during which I forgot the words to my poem, I said “Dad-gum.” Time to get into the birth tub. Ah, the birth tub. Bliss. I could drape over the sides and flip my Hypnobabies light switch to “off.”
Using hypnosis, I totally kicked transition’s butt. Oh yeah. Smiling and relaxing, this birth was a piece of cake. Until at 1pm, I swore again. Scott notes that I said “Yowzers.” (Ahem, Kelley are you reading? I will never pick on you again).
I should interject that Cedar was sounding beautiful. She was actively involved and had a great heart rate the whole time. Never gave us a worry.
I began feeling a little pushy. I was really looking forward to pushing. My firstborn, Norah, was so easy-breezy to push (although her 32 hour labor was challenging). I pushed Norah out in 20-something minutes with barely a sound. Ah, but Cedar. My first tentative push with Cedar told me something was different. And I began to fear. Fear+birth=pain. What was I afraid of? Well the doula brain was happy to rush back into high gear and tell me. I was afraid of a posterior baby. A nuchal hand. Tearing. Having to transport for suturing. Shut up, thinking brain!
Scott got into the tub at 1:20 and I tried pushing a few times while standing up. Then squatting. Both were overwhelming in sensation. I birthed Norah while squatting and I was barely aware of her descent. In fact, she took all of us by surprise when she tumbled out in between contractions. Cedar. Oh Cedar. First to present was the bag of waters–yep, still intact. I felt it with my hand and it was so hard. Until it broke–nice gush of clear fluid. Then, I felt Cedar descending like a freight train. I was on my knees but moved to a knee-crouch kind of position. Really, I think I was crouched because I was contemplating jumping out of the tub and just running away. Scott applied counterpressure to my perineum. I put pressure on my front and around the head. Wow, the sensations were incredible. And not incredible like orgasmic birth incredible. Nope, none of that. Scott said something later about feeling the energy and power of my uterus. He said birth should be an olympic sport because of that powerful muscle.


Cedar was born at 2:18. Scott caught her and brought her to the surface. She was not posterior. No nuchal hand. And I did not tear. On my chest, I rubbed her and snuggled her. She looked so healthy. And she was. I didn’t want to look to see if she was a girl or boy. That took some time.

After the placenta came, Scott clamped and cut the cord. No one noted the time but I know Cedar was already nursing by then. We got out of the tub. I drank some OJ. We examined Cedar (heart rate, respiration, temp, etc). Unfortunately, my bleeding was a bit heavy and my uterus was not clamping down as well as it could have. So I got a shot of pitocin, took some herbs, and had lots of “fun” fundal massage to get my uterus to contract.
Cedar weighed in at 8lbs 10oz and was 21 inches long.
Then we all went to bed. And I pretty much stayed there for 5 days. Snuggling and nursing and being visited by lovely family and friends. The great Cassandra even came the next day to give me an acupuncture treatment! And sweet midwives-to-be Carey and Crystal picked up my placenta the next day and encapsulated it for me. I also discovered how wonderful coconut water is for restoring electrolytes. More about amazing placentas and postpartum time later.
Fini.



 I promise to post a full birth story in a few days with strange details like how “The Love Song of J. Alfred Prufrock” played into my labor and how my stomach kept growling while I birthed. And how I kept trying to doula myself–not a good thing.
I promise to post a full birth story in a few days with strange details like how “The Love Song of J. Alfred Prufrock” played into my labor and how my stomach kept growling while I birthed. And how I kept trying to doula myself–not a good thing. I’m 24 weeks or is it 25? I don’t remember. I usually cheat and hop over to
I’m 24 weeks or is it 25? I don’t remember. I usually cheat and hop over to 